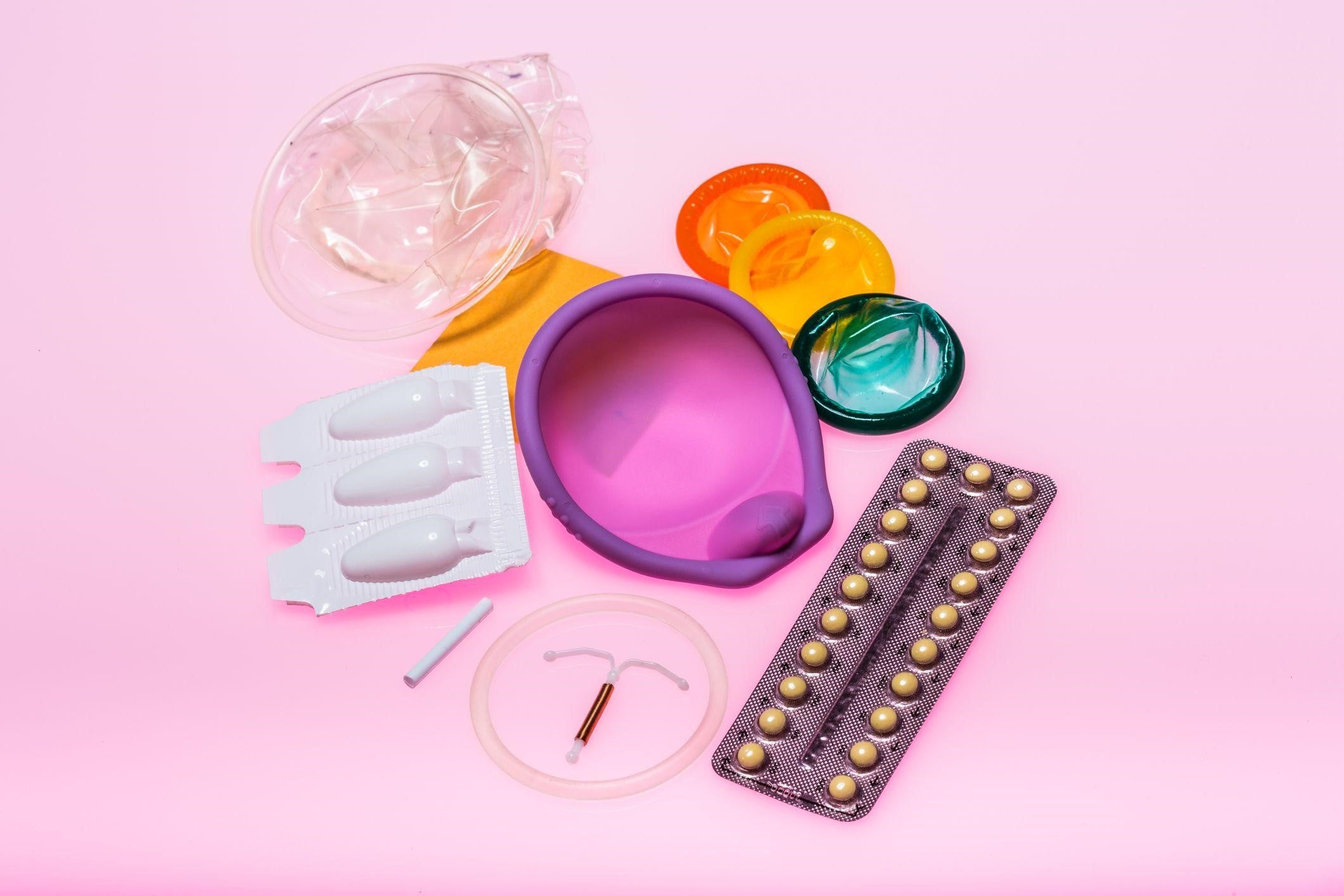
This is a question I get asked over and over - which contraception is right for me?
Contraceptives are used for reasons other than preventing pregnancy - for example - for regulating menstrual cycles, for reducing pain in endometriosis, to reduce heavy blood loss, to treat acne......there is a long list!
However, for the purposes of this blog, I'm simply looking at which method is best for you when making your choice to prevent a pregnancy. If you didn't use contraception at all, 85 women per year would get pregnant! (1)
There are a range of different contraceptive options for women currently available in the NI. (Disappointingly, there are only 2 options for men - vasectomy and condoms) The type that works best for you will depend on your health and circumstances.
There are several issues to consider when deciding which method of contraception is right for you (and your partner). But remember - preventing pregnancy is not the only issue when deciding your contraceptive. The only way to prevent STI's is to use a condom.
The contraceptive choices is a great website and I'll link it here

Here are some of the questions I would ask myself before commencing on contraception
Do you want regular periods, or no periods?
Do you want lighter/less painful periods?
Do you want less acne?
Do you want less PMS?
Do you want something that is less effort to remember?
- The answer to these questions will determine what type of contraceptive is best for you. For example, if you know you will forget to take a pill regularly the coil, the injection, the implant or the weekly patch may be better for you.
- So lets look at what is available.
- As there are so many types of contraception, you might want to watch this video, or just skip to the method that interests you the most! And I summarise it all in the blog!
The combined contraceptive pill
Otherwise known as 'the pill'!
The combined pill (‘the pill’) is taken every day, usually with a week off once a month (for a period). But see myths below!
It contains two hormones which are very similar to the body's own hormones.
Taken correctly it is 99% effective, but occasionally it is not taken correctly. In real terms, 9 women will become pregnant every year while on the mini pill (1)
Easy to start and stop, but can be difficult to remember to take it. The combined pill is also very useful for regulating periods, and reducing heavy blood loss.
Myths about the combined pill
Most people don’t put on weight
Sometimes the pill makes people feel more hungry. Studies show that most stay the same weight – 1 in 10 put on weight, and 1 in 10 lose weight while they are on the pill.
Some users notice bigger breasts
You don’t need a break from the pill
It’s safe to take from teenage years up to the age of 50 (for most people). It’s fine to have been on the pill from a young age, and for many years – there is no need for a break
You don't need to take it at the same time every day
It's good to have a routine which reminds you to take the pill, but it works fine if a pill is taken once a day, at any time
Not all pills suit everyone
One pill might suit someone really well, and another might cause moodiness, hunger, nausea, or less desire for sex. Everyone is unique, and there are different kinds of pills available, so it’s worth trying a few different brands of combined pill to find one which suits
You don’t need to have a period once a month
It’s safe to miss periods by taking several packets in a row without a break – blood doesn’t build up inside, because the womb lining stays thin. It can help people feel more energetic if they are not losing iron each month in a period.
The pill does not cause infertility
When people come off the pill, fertility returns to normal, meaning that it’s possible to get pregnant within a few days or weeks. It’s important to know that it’s less easy to get pregnant as you get older – it’s harder to get pregnant over the age of 35. (1)
For pros and cons of the combined pill click -
Combined Pill | Contraception Choices
One draw back is the slightly increased risk of a blood clot. I discuss this in the following video, and why attending your yearly pill check is so important.
https://youtube.com/shorts/sBhzzCUOlxo?feature=share
Most people will go to their GP to get the contraceptive pill, but you can also get it from the family planning clinic.
The Mini Pill (progesterone only pill)
The progestogen-only pill (the mini-pill) is taken every single day without any breaks. Taken correctly it is 99% effective, but occasionally it is not taken correctly. In real terms, 9 women will become pregnant every year while on the mini pill (1)
It contains a hormone which is very similar to the body's own hormones.
It needs to be taken at roughly the same time every day.
The major difference between this pill and the combined pill is that the mini pill does not contain oestrogen. It only contains progesterone. It is just as effective as the normal pill, with just a few draw backs.
The main draw backs are that in the beginning, when a woman starts it, it may cause bleeding. However, for most people, this isn't an issue, and in fact you may not bleed at all on this pill, as you take it all month long. So on the flip side of this, it may be useful for ladies with heavy bleeds.
One other draw back is, it also needs to be taken at roughly the same time every day.
One major benefit of this pill is that its much safer to use this in women at risk of blood clots. Oestrogen increases blood clot risk. As there's no oestrogen in this pill, it is safer in women at risk.

Women at higher risk of blood clots are
-over 35 years
-BMI >30
-Raised BP
-Smoker
-Previous blood clot (2)
In 2014, the European Medicines Agency (3) reported that they would expect between five and 12 blood clots to occur among 10,000 women who take combined contraceptives for one year. By comparison, they would expect to see two cases of blood clots among 10,000 women not using these contraceptives.
So your risk of getting a blood clot with the pill are low, but if you are taking the progesterone only pill, your risk is the same as someone not taking any medication. The risk of blood clots is largely only associated with the combined pill!

You can also buy the progesterone only pill over the counter in your community pharmacy.
Click on this link on our instagram page to find out more
N Ireland Pharmacy of Year 2023 (@melvinpharmacy) | Instagram
The Injection

The injection (or depo) is given as an injection into the bottom or thigh every three months. It must be given by a registered GP or nurse.
It contains a hormone called progestogen which is very similar to the body's own hormones.
Its long-lasting and convenient - as women don't need to be reminded to take it, it can stop periods temporarily. It is effective, and approx 3 in 100 women using it will become pregnant in one year.
One of the great advantages about the injection is that it lasts 3 months. Being progesterone based, like the mini pill, it can be useful in stopping heavy periods. 1 in 4 women will experience no bleeding at all while on it.
The main disadvantage is it can reduce bone turnover, meaning your bones can become more brittle while you use it - so should not be used in women at risk of osteoporosis. Also, it does take time to wear off, so not ideal if you are planning a baby in the near future. It is important women take this into account, although there's no evidence it reduces fertility. (1)
Most people will be able to get the injection from their GP, or the family planning clinic.
The contraceptive injection - NHS (www.nhs.uk) (4)
The Patch

The patch is a square sticker like a thin plaster and sticks on to the skin. Very useful for women who don't like swallowing tablets. It is highly effective is used correctly - but similar to the pill, that is not always the case. 9 in 100 women will become pregnant while using the patch every year (1)
This skin absorbs two hormones (oestrogen and progestogen) which are very similar to the body's own hormones.
The patch is changed once a week. Its very similar in profile to the combined pill, other than it is applied to the skin. It is a light patch however, which means it may not be as discreet on darker skin.
The patch usually stays on well, even in the bath, shower, or sauna but needs to be put onto skin which is completely dry, with no moisturiser on.
It can be a nuisance to remember to change it. However, there is no requirement to take a patch free week anymore, the same as the combined pill, and changing it on the same day each week without taking a break can be helpful for some women. (1)
For more info on the patch, follow this link
Contraceptive patch - NHS (www.nhs.uk) (5)
The Implant
The implant is a soft piece of plastic that's put in under the skin of the arm.
It contains one hormone (a progestogen), which is very similar to one of the body's own hormones.
It lasts for 3 years, but can be taken out at any time. It is highly effective, and less than one woman a year will become pregnant when they are on it. (1)
Some people love the implant, and others don't get on with it at all.
The implant is incredibly convenient and can help period pain and heavy bleeding.
Periods can change a lot. Many find their periods become less frequent or lighter. One in four people won’t have any periods at all, and about 1 in 5 will have periods or light bleeding (spotting) that's irregular, or have heavier bleeding that becomes a nuisance. Changes in periods won't cause any harm and won't stop you getting pregnant in future.
It’s put in under the skin of the upper arm by a trained doctor or nurse and lasts for 3 years. There's a sharp jab from a small injection of local anaesthetic, and then it's not painful when it's put in.
You can get a prescription for the patch from your GP or the family planning clinic. (1)
For more information visit
Contraceptive implant - NHS (www.nhs.uk) (6)
The Copper Coil

The copper coil (or IUD) is made of plastic and copper. (There are 2 types of coils, a copper coil which is hormone free, and a coil that contains hormones - and it is dealt with later on).
It's put into the womb by a doctor or nurse, and lasts up to 5 to 10 years.
The IUD is popular because it has no hormones.
The IUD is great if pills are a nuisance to remember
It lasts up to 10 years, and is not affected by other medicines, vomiting or diarrhoea. It is highly effective, and less than one woman a year will become pregnant when they are on it. (1)
The IUD does not cause infertility
Fertility returns to normal after having the IUD taken out. It’s important to know that it’s less easy to get pregnant with age – it’s naturally harder to get pregnant over the age of 35
You can't feel the IUD during sex
Some partners do notice the threads during sex, but the threads can be trimmed so they are out of the way
The IUD is very discrete
The pattern of periods is not affected by the IUD.
If periods are heavy or painful, this can be treated by medication from a GP
The IUD can come out especially after periods in the first three months (1 in 20 chance)
In NI this form of contraception is usually fitted by a doctor in a family planning clinic. It is not routinely done in GP surgeries, unless the GP has done extra training in this area.
For more information on the copper coil see
Intrauterine device (IUD) - NHS (www.nhs.uk) (7)
Fertility Awareness (Natural Family Planning)

Fertility awareness (natural family planning) is a way of predicting ovulation, to work out when pregnancy is more likely
The method involves recording signs of fertility such as body temperature, thickness of fluid in the vagina, and calculating fertile times from menstrual cycle dates.
Teaching from a qualified fertility awareness teacher is recommended.
Fertility awareness can be very effective (with daily monitoring)
Fertility awareness methods require close attention to patterns over time.
Monitoring involves recording body temperature first thing in the morning, feeling the thickness of fluid in the vagina, and recording the pattern of periods, to work out when it is likely that an egg will be released (ovulation). Fertility awareness is more effective when two or more of these signs of fertility are monitored.
You need to record patterns for at least three months before starting to rely on predicting the fertile days. If periods are irregular, or if you have recently stopped using a hormonal method of contraception, it takes longer to be able to predict fertile times accurately.
Fertility awareness does not work if hormones are taken at the same time, because the hormones will alter all of the signs of fertility.
There are fertility charts and mobile phone apps that can help track the changes and to predict fertile days.
To be effective, unprotected sex must be avoided around the most fertile days. This means typically avoiding unprotected sex for 8-9 days in a month, to allow for the time that sperm can survive, added to the time that an egg can survive.
It is not a preferred method to prevent pregnancy as 24 women per 100 in any one year will become pregnant using this method. It is a great way of ammping however if you would LIKE to become pregnant (1)
The Hormonal Coil
The hormonal coil (or IUS) is made of plastic and releases a small amount of progestogen hormone which is similar to one of the body's own hormones. It is different to the copper coil as its hormone based.
It is highly effective, and less than one woman a year will become pregnant when they are on it. (1)
It's put into the womb by a doctor or nurse and lasts up to 6 years. It is a highly effective contraceptive, and the one that is recommended by the NHS.
The IUS can be wonderful in helping heavy or painful periods - more so than the copper coil.
Otherwise, it is very similar to the copper coil, except it has progesterone. The major difference between the 2 is how the prevent contraception.
One major positive for the hormonal coil is that it can be used as the progesterone part of HRT.
In addition, If you're 45 or older when you have the IUS fitted, it can be left in until you reach the menopause or no longer need contraception.
In NI this form of contraception is usually fitted by a doctor in a family planning clinic. It is not routinely done in GP surgeries, unless the GP has done extra training in this area.
For more information on the hormonal coil see
Intrauterine system (IUS) - NHS (www.nhs.uk) (8)
The diaphragm
Diaphragms and cervical caps are cups made of silicone.
It is put at the top of the vagina, to cover the cervix (neck of the womb).
It's used with spermicide (a cream that kills sperm), and necessary to check it's in the right place before sex. Their effectiveness really depends on the user.
Diaphragms and caps have no hormones. You need to check whether the diaphragm is in the right place in the vagina - this is usually easy to learn.
Caps and diaphragms can be obtained from family planning clinics and you will be showed how to use them. They are available in different sizes and it's important to get one which covers the cervix and sits comfortably inside.
You need to learn how to check whether the diaphragm is in the right place (feeling for the cervix with a finger in the vagina).
Diaphragms and caps need to be cleaned after use with soap and water, rinsed, and left to dry. They should be checked for holes or signs of damage before use.
You may need to change diaphragm size after gaining or losing weight, or having a pregnancy.
They need to be put in before sex and left in for at least 6 hours afterwards.
When used perfectly, diaphragms and caps are about 94% effective – meaning that if 100 people used a diaphragm or cap for a year, about 6 of them will have an unplanned pregnancy. However, allowing for the ups and downs of life, the average user can expect them to be around 88% effective – meaning that if 100 people used a diaphragm or cap every day for a year, about 12 of them will have an unplanned pregnancy. (1)
For more information please click on this link
Contraceptive diaphragm or cap - NHS (www.nhs.uk) (9)
Contraceptive ring

The ring is a soft plastic ring put in the vagina.
It releases two hormones (oestrogen and progestogen) which are similar to the body's own hormones. Similarly to the patch and the pills, approximately 9 women per 100 will become pregnant in any one year using this method (1)
Each ring lasts for three weeks.
The ring is easy to put in
It finds a comfortable position, and doesn't need to be put anywhere particular in the vagina. It's just a different way of absorbing the hormones
Unlike the pill, the ring still works if you have sickness (vomiting) or diarrhoea.
The ring may ease premenstrual symptoms, and bleeding will probably be lighter and less painful.
The ring can also be used to treat menopausal symptoms, like hot flushes and vaginal dryness in people under 50.
The contraceptive ring is available on prescription from your doctor.
For more information please visit
Vaginal ring - NHS (www.nhs.uk) (10)
Male and Female Condoms
There are two different types of condoms, condoms which are worn on the penis, and condoms which are worn inside the vagina.
Condoms are made from a very thin latex, synthetic nitrile, polyisoprene or polyurethane, and can be used for vaginal, oral and anal sex.
The size and fit of condoms on a penis is important so that they are comfortable and don't break or slip off.
Condoms are the only option that prevents pregnancy and STIs. You cannot get them from your doctor, but you can get them free of charge from the Family Planning Clinic. Condoms are less effective at preventing pregnancy than other contraceptives - approx 15 in 100 women relying solely on condoms will become pregnant in a given year. However, the are vital for preventing Sexually Transmitted Diseases. As STD's are on the rise, everyone who is sexually active and has more than one partner and not had an STI check, should be using a condom and another contraceptive as part of their contraceptive choices.
Did you know?

Condoms have expiry dates. They can also weaken in different conditions, such as in hot places or in sunlight.
Two is not better than one- doubling up and using two condoms at the same time actually increases the chances of the condoms breaking. (1)
For more information on condoms please visit
Female condoms - NHS (www.nhs.uk) (11)
Condoms - NHS (www.nhs.uk) (12)
Withdrawal Method
Withdrawal (pulling out) is when the partner pulls out before ejaculation.
It Suits some couples.
1 in 5 (~20%) risk of pregnancy.
If you're keen to avoid hormones, contraception methods like the copper coil or diaphgram might be more suitable because they are more effective. You can still have skin to skin contact with a partner with these methods
Health professionals do not recommend withdrawal as a form of contraception.
We've now looked at all the types of reversible contraception available - permanent contraception is male and female sterility.
Don't forget, now that you've seen all the different types of contraception available - click here to determine which is right for you
www.contraceptionchoices.org
Here's the difference between all the methods at a glance - (taken from contraceptionchoices.org)

In summary we have looked at all the forms of contraception available, and the one choice does not fit all. There will always be factors that will need to be taken into consideration. For example, am I a clot risk? Do I want to be able to get pregnant straight away when I stop contraception? Do I remember to take tablets? Am I on other medication?
This blog cannot cover all these questions, but it can give you a brief over view of each method. Within each method there are varying choices also - for example, there are loads of 'pill' and mini pill options. The contraceptive choices website is a great place to start your research www.contraceptionchoices.org but you can always pop in and speak to your pharmacist or your GP
I hope you have found this informative!
(1) Effectiveness | Contraception Choices
(2) www.fsrh.org
(4)The contraceptive injection - NHS (www.nhs.uk)
(5) Contraceptive patch - NHS (www.nhs.uk)
(6) Contraceptive implant - NHS (www.nhs.uk)
(7) Intrauterine device (IUD) - NHS (www.nhs.uk)
(8) Intrauterine system (IUS) - NHS (www.nhs.uk)
(9) Contraceptive diaphragm or cap - NHS (www.nhs.uk)
(10) Vaginal ring - NHS (www.nhs.uk)