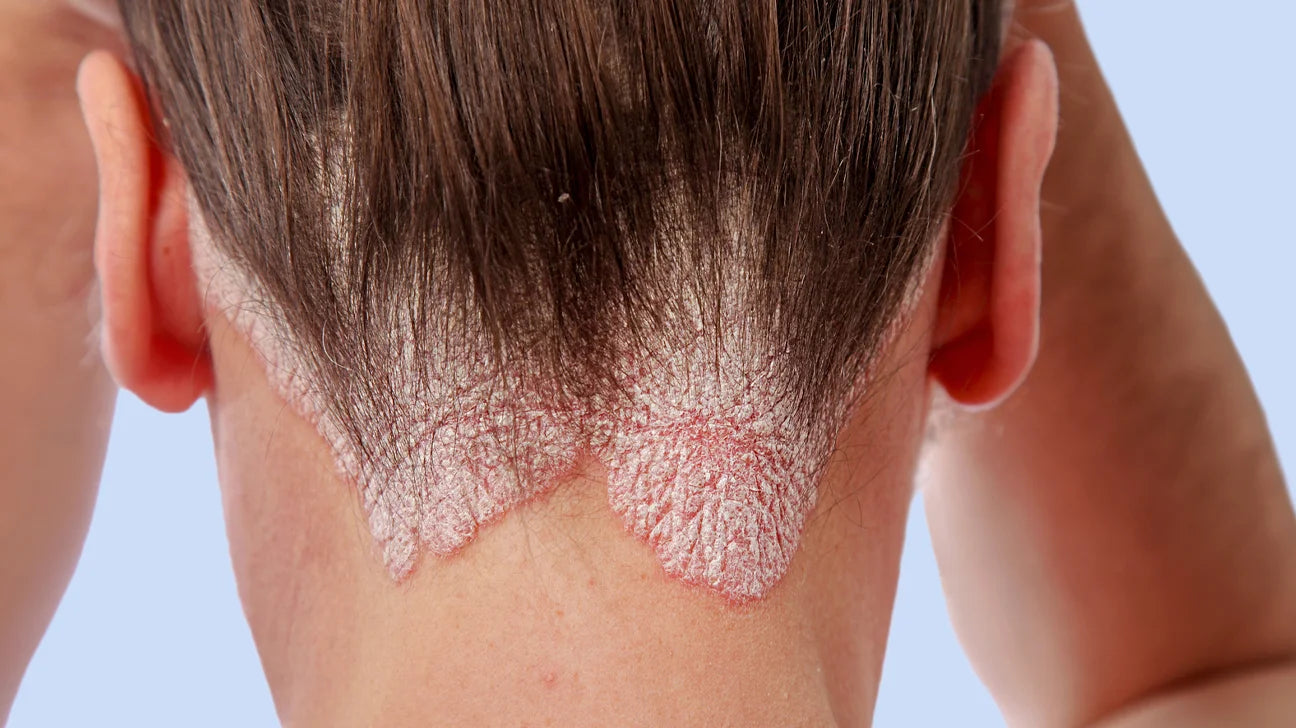
Currently affecting up to three per cent of the UK population, psoriasis is an inflammatory skin disease that typically follows a relapsing and remitting course. Pharmacist Timothy McClure takes a closer look into this distressing condition.

What is Psoriasis?
Psoriasis is characterised by scaly skin lesions which can be in the form of patches, papules or scaly plaques. They can occasionally be sore. Itch is often a feature (2) Psychological and social effects are common and can be profound. Psorasis is non contagious, however the condition is chronic and long-term with periods of remission and relapse. (1,2)
Although there is no cure, it is important to remember that psoriasis can be managed and with the right treatment and advice, the impact on quality of life can be minimised.
Psoriasis can present at any age, but is more likely to first present between 15 years and 30 years of age. It is uncommon in children with a prevalence of under one per cent in most studies. While men and women are equally affected, psoriasis is more common in Caucasians.(2,3)

The skin lesions of psoriasis are a consequence of hyperproliferation of the epidermis - this means the skin cells divide much more rapidly than normal. Subsequently, the body can take just a few days to replace skin – a process that normally takes around 28 days. This accumulation of skin cells builds up to form raised psoriatic plaques on the skin. In addition, inflammatory cells increase in number. (1,2)
What causes Psorasis?
The cause of increased cell turnover and skin inflammation in psoriasis is not known. Genetic factors appear to be involved with around one third of sufferers having a close relative also affected. Several factors are however believed to affect the onset or exacerbation of the disease. These include:
- Streptococcal throat infection
- Drugs (examples include lithium, beta-blockers, antimalarials, non-steriodal anti-inflammatories and angiotensin-converting enzyme inhibitors)
- Trauma (known as the Koebner reaction, the development of psoriatic plaques can follow injury to the skin 7 to 14 days post trauma)
- Sunlight (though beneficial in most cases, may make psoriasis worse in a small number of people)
- Psychological stress
- Post-partum hormonal changes
- Smoking
- Excessive alcohol intake (1,3,5)
Types of Psorasis

There are several different types of psoriasis. Many people have only 1 type at a time, although you can have 2 different types together. One type may change into another or become more severe.
Most cases of psoriasis go through cycles, causing problems for a few weeks or months before easing or stopping.
Chronic plaque psoriasis
Chronic plaque psoriasis (including scalp, flexural psoriasis) is the most common form affecting 80 – 90% of people with psoriasis. Psoriatic plaques are distinctively raised, red in colour, irregular to oval in shape, one to several centimeters in size and are well defined with sharply demarcated boundaries. The plaques typically have a dry, thin, silvery-white scale on top. Plaques can occur anywhere on the body, but are most often located over the elbows and knees, on the scalp, and lower back. Smaller plaques, especially in the leg and sacral regions, may coalesce into larger lesions. The face is rarely affected. Chronic plaque psoriasis is often itchy but does not usually cause excessive discomfort. (1,2)
Around 50% of those with chronic plaque psoriasis affecting their body will also have psoriasis affecting their scalp, however it may occur alone in some people. Leading to hair loss in severe cases, scalp psoriasis may affect the whole scalp or just a partial area.
Pustular psoriasis
The second most common form of psoriasis is pustular psoriasis. Typically affecting only the palms of the hands or soles of the feet, this form of psoriasis is characterised by patches of very red or dark skin, covered with small yellow/brown pustules. The fluid within the pustules does not contain bacteria and is not contagious. The skin around the pustules is often thick, flaky and prone to cracking. Consequently pustular psoriasis can be painful, making the use the hands or walking difficult. Pustular psoriasis localised to the palms and soles is more common in women than in men (ratio of 9:1) and although it can present at any age, it usually occurs in the fourth or fifth decade of life. (1,2)

Generalised pustular psoriasis is relatively rare but is a serious condition and requires urgent medical attention. It presents with rapidly developing widespread redness, followed by the eruption of small pustules on any part of the body. The skin often feels hot to the touch and may be sore, tender or itchy. Systemic illness often occurs. The precise cause of generalised pustular psoriasis is unknown, but potential triggers are thought to include sudden withdrawal of steroids, infection, certain medications or exposure to ultraviolet light. (1)
Nail psoriasis

Nail psoriasis can affect up to fifty per cent of patients with psoriasis. Although commonly seen alongside skin psoriasis, nail psoriasis can occur alone and may go through phases of exacerbation. Signs and symptoms can occur on either fingernails, toenails or both. Nail psoriasis can be easy to misdiagnose as a fungal infection as many of the signs are similar. An affected nail will generally lose its natural shape and feel, with pitting occurring across the surface. Yellow/orange discolouration, nail thickening and onycholosis (detachment from the nail bed) are also common features. In moderate to severe cases, nail psoriasis can be painful making the use of hands and feet difficult. (1,2)
Guttate psoriasis
Owing to its small (<1cm) round or oval plaques, guttate psoriasis is also referred to as ‘drop’ psoriasis. Guttate plaques are often bright pink or red on fair skin types. Some fine scaling may also be present. (1) Plaques are widespread, usually occurring in large numbers across the torso, back and proximal limbs. Lesions can also occur on the face, ears and scalp but it is rarely seen on the soles of the feet. (2)

Guttate psoriasis can occur at any age, but is more common in children and adults younger than 30 years of age. It is often triggered by a streptococcal throat infection. This form of psoriasis is self-limiting and typically resolves within 3 - 4 months of onset. It can occur as a first presentation of psoriasis or as an acute exacerbation of plaque psoriasis. Although long-term prognosis is unknown, it is estimated about a third of people with guttate psoriasis develop chronic plaque disease.1,2
Erythrodermic psoriasis
Causing erythromderma (generalised redness of the skin), erythrodermic psoriasis is a rare but dangerous form of psoriasis requiring urgent medical treatment. This form of psoriasis spreads rapidly to typically encompass over 90% of the skin's surface. Characteristically the skin is red and hot with the dermatological characteristics of psoriasis often lost. Scale is usually finer and flakier than the classic silvery scale of plaque psoriasis. The patient can quickly become systemically unwell as the condition interferes with thermoregulation. This can result in excessive protein and fluid loss, leading to dehydration, heart failure and severe illness. Onset can occur acutely over a few days or weeks, or gradually evolve over several months from pre-existing psoriasis. (1,2)
Psoriatic arthritis
Around ten to twenty per cent of people with chronic plaque psoriasis will develop psoriatic arthritis. Any joint can be affected but it most commonly affects the joints of the fingers and toes. Any patient presenting with these symptoms should be referred to their GP. (1)

Treatments
Emollients
Emollients are moisturising treatments applied directly to the skin to reduce water loss and cover it with a protective film. If you have mild psoriasis, an emollient is probably the first treatment your GP will suggest.
The main benefit of emollients is to moisturise the skin and reduce itching and scaling. Some other topical treatments are thought to work better on moisturised skin. Wait at least 30 minutes before applying another topical treatment after an emollient.
Emollients are available as a wide variety of products and can be bought over the counter from a pharmacy or prescribed by your GP.
Steroid creams or ointments
Steroid creams or ointments (topical corticosteroids) are commonly used to treat mild to moderate psoriasis in most areas of the body. The treatment works by reducing inflammation. This slows the production of skin cells and reduces itching.
Topical corticosteroids range in strength from mild to very strong. Only use them when recommended by your doctor.
Stronger topical corticosteroids can be prescribed by your doctor and should only be used on small areas of skin or on particularly thick patches. Overusing topical corticosteroids can lead to skin thinning.
Vitamin D analogues
Vitamin D analogue creams are commonly used along with or instead of steroid creams for mild to moderate psoriasis affecting areas such as the limbs, trunk or scalp. They work by slowing the production of skin cells. They also have an anti-inflammatory effect.
Examples of vitamin D analogues are calcipotriol, calcitriol and tacalcitol. There are very few side effects as long as you do not use more than the recommended amount.
Calcineurin inhibitors
Calcineurin inhibitors, such as tacrolimus and pimecrolimus, are ointments or creams that reduce the activity of the immune system and help to reduce inflammation. They're sometimes used to treat psoriasis affecting sensitive areas, such as the face, the genitals and folds in the skin, if steroid creams are not effective.
These medications can cause skin irritation or a burning and itching sensation when they're started, but this usually improves within a week.
Coal tar
Coal tar is a thick, heavy oil and is probably the oldest treatment for psoriasis. How it works is not exactly known, but it can reduce scales, inflammation and itchiness.
It may be used to treat psoriasis affecting the limbs, trunk or scalp if other topical treatments are not effective.
Coal tar can stain clothes and bedding and has a strong smell. It can be used in combination with phototherapy.
Dithranol
Dithranol has been used for more than 50 years to treat psoriasis. It has been shown to be effective in suppressing the production of skin cells and has few side effects. However, it can burn if it's too concentrated.
It's typically used as a short-term treatment, under hospital supervision, for psoriasis affecting the limbs or trunk, as it stains everything it comes into contact with, including skin, clothes and bathroom fittings.
It's applied to your skin (by someone wearing gloves) and left for 10 to 60 minutes before being washed off.
Dithranol can be used in combination with phototherapy.
In what order are these treatments given

NICE recommend short term intermittent use of a potent topical corticosteroid (e.g. betamethasone) or a combined potent topical corticosteroid plus a Vitamin D analogue to gain rapid improvement in plaque psoriasis. Short term intermittent use of a potent topical corticosteroid applied once daily is recommended in scalp psoriasis. If there is a poor initial response, a combined topical preparation containing a potent corticosteroid and a vitamin D analogue can be trialled for up to four weeks. Moderate potency topical corticosteroids (e.g. clobetasone) are recommended for short term use in facial and flexural psoriasis for up to two weeks. (5)
For severe, resistant, unstable or complicated forms of psoriasis, ultraviolet light therapy and systemic treatments including methotrexate, ciclosporin and acitretin can be initiated under specialist supervision in secondary care. (4)
Living with Psorasis
Psoriasis is different for each person. For some people it may not have a huge impact on day-to-day life, but for others its impact can be significant. For those who find their day-to-day lives are affected, we know that many things can be disrupted by psoriasis, from work to relationships, getting a good night's sleep to wearing what you want.
If you have psoriasis, you may find the following advice helpful.
www.psoriasis-association.org.uk/living-with-psoriasis
Psorasis and Self Care
Self care is an essential part of your daily life. It involves taking responsibility for your own health and wellbeing, with support from those involved in your care.
Self care includes staying fit and a healthy weight, maintaining good physical and mental health, preventing illness or accidents, and caring more effectively for minor illnesses and long-term conditions.
People with long-term conditions can benefit enormously from self care. They can live longer; have less pain, anxiety, depression and fatigue; have a better quality of life; and be more active and independent.
Click here for more advice.
https://www.papaa.org/learn-about-psoriasis-and-psoriatic-arthritis/diet-and-lifestyle/
https://www.psoriasis-association.org.uk/itching
Useful Links
www.psoriasis-association.org.uk
https://www.papaa.org This site has a great symptom checker
https://www.nhs.uk/conditions/psoriasis/
References
1. Psoriasis Association UK. https://www.psoriasis-association.org.uk/psoriasis-and-treatments/ [Online]
2. Patient UK. Psoriasis. https://patient.info/health/psoriasis-leaflet [Online]
3. British Association of Dermatologists. Psoriasis – An Overview. http://www.bad.org.uk/shared/get-file.ashx?id=178&itemtype=document [Online]
4. British National Formulary Issue 73.
5. NICE Psoriasis: Assessment and Management CG153. https://www.nice.org.uk/guidance/cg153 [Online]